The end of the year is approaching and so are your ACA Reporting deadlines. Make sure to review your Compliance Alerts for the year in preparation for ACA Reporting.
The ACA Manager tool creates a Compliance Alert whenever it detects a coverage issue. To check for them:
- Login to your account.
- Navigate to the My Reports Tab → ACA (Affordable Care Act)→ ACA Data Summary
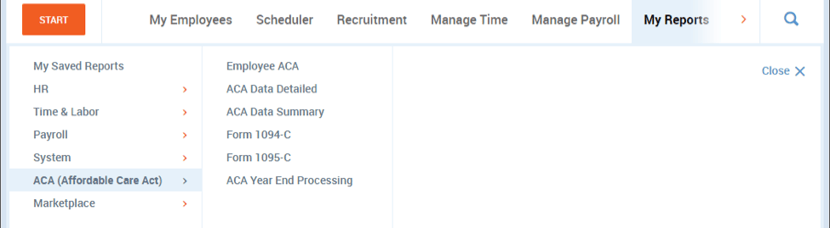
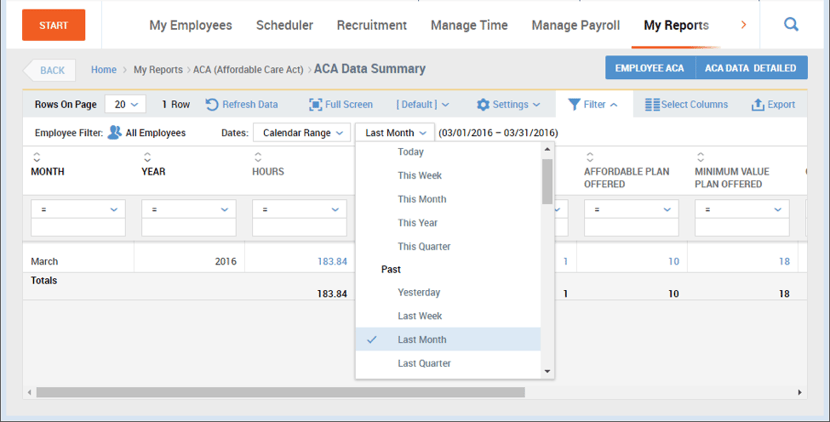
- While in the report, change the date to reflect the entire year.
- Once the page is refreshed, look under the Compliance Alert column (eighth from the right). Each month will have a blue number listed.
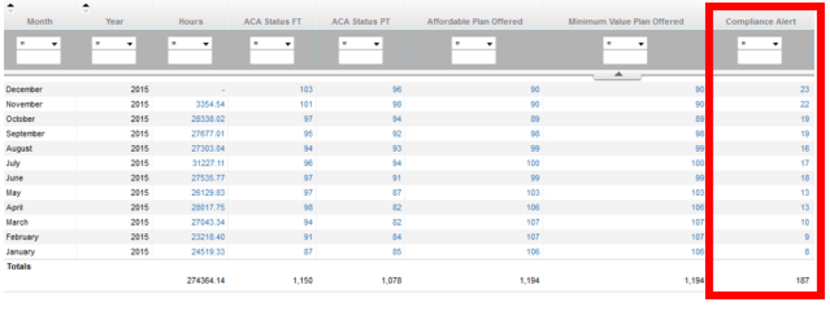
- Clicking on the blue numbers will open up a new report listing anyone with a Compliance Alert.
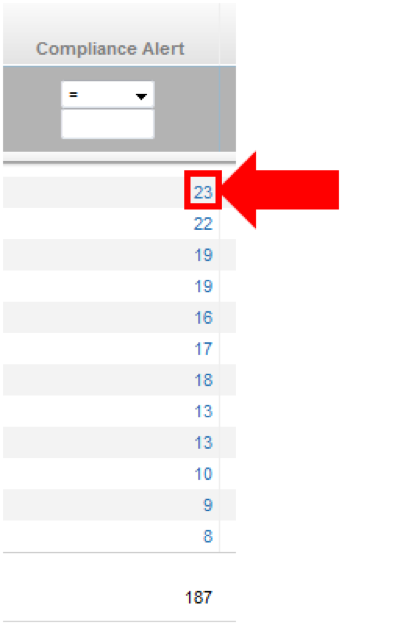
3 Reasons Your Account Might Have Compliance Alerts
- The employee waived coverage but the waiver did not get added as a Benefit Plan/Benefit Profile to the system. Maintaining current waivers (and updating the ACA Manager with that information) is an extremely important step in compliance. IRS Form 1095-C for the employee who waived coverage will have a code reflecting that the employee was offered coverage. Keep waivers documented and the system updated!
- The Benefit Profile did not get assigned to the employee or did not have correct dates. If the employee has health insurance all year, assign a Benefit Profile to reflect that. If the employee started receiving insurance mid-year, ensure those dates are represented correctly. Please refer to our training videos for more information on how to correctly date the Benefit Profile.
- The employee was not offered coverage but should have been. Under ACA, employees are considered non-variable, or full-time, if they average 30+ hours per week or 130+ hours per month. Any employee coded as variable, or part-time, but working full-time hours will trigger a Compliance Alert.










